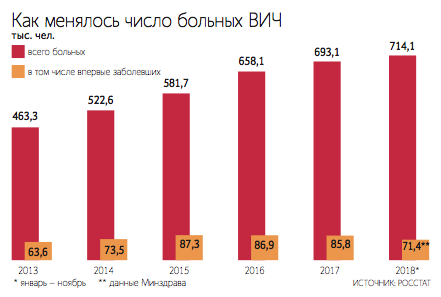
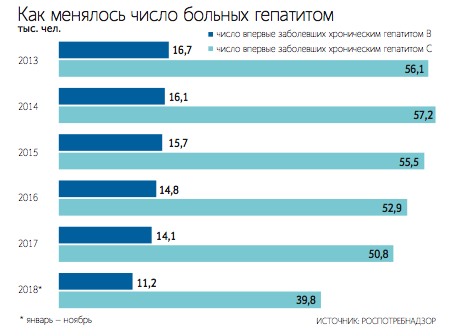
The number of new cases of HIV infection in Russia has been growing again. In 2022, 63,150 people were diagnosed with HIV, while a year earlier this figure was 61,098 people, according to the Russian Health Ministry. During the pandemic, fewer cases of HIV infection were detected in Russia due to reduced testing coverage and lockdowns.
The HIV detection rate in Russia increased by eight percent per 100,000 people in a year. There was an even bigger jump in particular regions. Compared with 2021, this figure almost doubled in the Belgorod Region. It increased by 76% in the Kaluga Region, by 66% in Yakutia, and by 60% in Ingushetia and the Altai Republic.

However, the Health Ministry’s data encompasses only people who have registered as outpatients at AIDS centers. They do not reflect those who have tested positive for HIV, but were not registered. The number of such people is as high as twenty percent of all confirmed cases of infection, estimates Vadim Pokrovsky, head of the Epidemiology and AIDS Prevention Research Department at Rospotrebnadzor’s Central Epidemiology Research Institute. Nor does this figure include foreign nationals and anonymous positive tests.
In 2021, 1,138,000 people with a confirmed diagnosis of HIV diagnosis resided in Russia. In 2022, another 60,000 people were diagnosed with HIV. To these groups we need to add around 300,000 people (according to Pokrovsky’s estimates) who have HIV but don’t know it because they haven’t been tested. Thus, the number of HIV-positive people in Russia is one and a half million, which is one percent of the country’s population.
2.6% of pregnant women in the Irkutsk Region are HIV positive.
At the Congress on Infectious Diseases, Pokrovsky said that almost a third of Russia’s regions are undergoing the generalized (third) stage of the HIV epidemic. He explained that there are three stages of the epidemic. The first (initial) stage involves isolated cases. The second (concentrated) stage occurs when more than five percent of any high-risk subpopulation is infected (for example, prison inmates, drug addicts, or sex workers, while the third (generalized) stage occurs when more than one percent of pregnant women are infected with HIV.
According to Pokrovsky, nine Russian regions are in the first stage of the epidemic, while forty-eight are in the concentrated stage, and twenty-seven are in the generalized stage. In the Irkutsk Region, 2.6% of pregnant women have been diagnosed with HIV, he noted. Ten percent of Russian prison inmates are infected with HIV, and four percent of Russian men over the age of forty have HIV, adds Pokrovsky.
In 2022, regions of Siberia and the Urals — Krasnoyarsk and Perm Territories, Orenburg, Kemerovo, Irkutsk, Tomsk, Chelyabinsk, Novosibirsk, Kurgan and Sverdlovsk regions — remained the leaders in the rate of HIV spread, as in previous years.
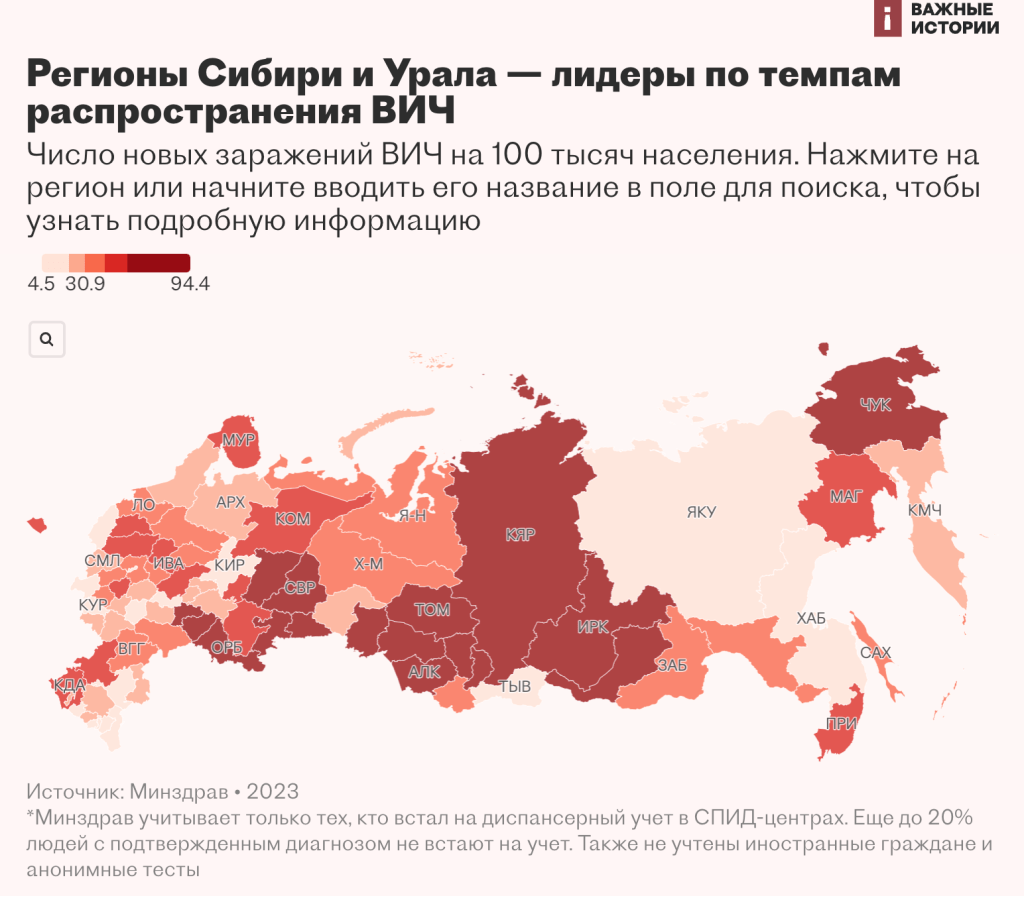
Click on the region or start typing its name in the search box to see specific figures.”
This map is interactive in the original article, as published on the Important Stories website.
And yet, flying in the face of its own data, which showed an increase in cases, in March of this year the Health Ministry reported a reduction in the number of new cases of HIV infection in 2022.
According to the UN strategy for eradicating HIV, a country should seek to hit the “90–90–90” treatment target if they want to beat the epidemic. This means that ninety percent of people with HIV should know their status, ninety percent of people who know they are HIV positive should receive sustained treatment, and ninety percent of patients undergoing treatment should have an undetectable (i.e., very low) viral load. When this is the case, an HIV-positive person undergoing antiretroviral therapy cannot transmit the virus to another person.
Antiretroviral (ARV) treatment is the principal means of combating HIV. Every person living with the immunodeficiency virus should receive this therapy. But that is not the case now.
In 2021, 82% of people who had regular medical check-ups and 56% of all those living with a confirmed diagnosis of HIV infection received ARV treatment, according to Rospotrebnadzor’s AIDS Prevention and Monitoring Center. An undetectable viral load was attained by eighty percent of those receiving ARV treatment.
The rest — more than half a million people with a confirmed diagnosis — do not receive treatment. Their viral load remains detectable, so they risk spreading the infection.
By law, Russian citizens should receive ARV treatment for free. However, the Health Ministry procures less medicine than HIV-positive people need, and has not increased the treatment budget despite the fact that the number of patients has been growing every year. Every day, the project “Interruptions.ru” fields messages from patients complaining about the unavailability of treatment.
49% of Russians registered as HIV positive are covered by drugs purchased by the state.
In 2021, Russia procured only 391,000 annual doses, according to the International Treatment Preparedness Coalition. This covers approximately 49% of the number of people who receive follow-up care, and 34.4% of all people registered as HIV-positive. Therapy coverage was thus fifteen percent lower in 2021 than in 2020.
The drugs procurement budget for 2023–2025 must be increased by at least fifteen billion rubles annually in order to provide all patients with the necessary treatment. However, the Finance Ministry is willing to allocate 31.7 billion rubles for drugs procurement annually during the period 2023–2025 — that is, it does not plan to increase spending.
And yet, according to one estimate, Russia spent ten trillion rubles on the war over the past year. This same amount of money could provide all Russians in need of it with ARV treatment for 270 years in a row.
The Health Ministry procures drugs for ARV treatment on the federal level, while the regions must purchase the drugs they lack themselves, an activist who helps people with HIV explained to Important Stories on condition of anonymity.
According to her, AIDS centers in the regions submit applications to the Health Ministry for the amount of drugs they need. But the Health Ministry buys less than requested — for example, AIDS centers might apply for ten thousand doses, but the Health Ministry buys them only seven thousand. The regions have to find the money to make up for the shortfall in drugs.
“We must increase the number of patients in treatment and increase coverage,” our source told us. “At the moment, it is unclear what to do without additional allocations of money for purchasing medicines.”
If the Russian authorities spent ten trillion rubles on medicines, rather than on the war in Ukraine, they could provide HIV-infected Russians with the treatment they need for 270 years in a row.
The regions are not required to buy additional medicines, nor do all of them do it. Consequently, patients find themselves in unequal conditions: in richer regions, they receive the appropriate treatment, while in poorer regions they do not. Moreover, spending on drugs does not depend on how bad the HIV epidemic is in a particular region. This can be seen by looking at procurements of the drug Dolutegravir. According to our source, it is a well-researched and rather expensive drug that is suitable for many patients. But the Health Ministry has been reducing its purchases of the drug, while the country’s richest regions — the Tyumen Region, Moscow, St. Petersburg, and the Khanty-Mansi Autonomous District — spent the most of their own funds on it in 2022.
More than half of Russia’s regions did not purchase additional Dolutegravir for their patients at all, including, for example, the Sverdlovsk Region, where almost three thousand new patients were registered in 2022.
More than 77% of the money spent on Dolutegravir was spent by regions where only 23% of new HIV patients live.
Cutting-edge HIV treatment is available mainly to residents of rich regions
More than 77% of the public funds spent on procuring the drug Dolutegravir in 2022 were allocated by regions where only 23% of new cases live

In 2022, Kommersant wrote about the reduction of purchases of expensive drugs for which there are no less-expensive substitutes. In 2021, such drugs accounted for 67% of the total volume of ARV treatment purchases, while in 2022, this figure was 55%. Cheaper drugs are being purchased to replace them.
Reducing the choice of drugs available makes it more difficult for patients to choose a treatment that suits them without causing side effects. It happens that only one drug out of four is suitable for a person, but the region where they live does not supply it.
Pokrovsky notes that the 63,000 new cases in 2022 is a high rate of infection. In reality, there are even more HIV-positive people in Russia, since the country’s most vulnerable groups are less likely to be tested.
“In part, the large number of new cases is due to the fact that we do test a large portion of the population: more than forty million tests were done in 2022. (But we must take into account the fact that, for example, pregnant women and donors are tested several times a year.) On the other hand, people who are particularly vulnerable to HIV infection — drug users and men who have sex with other men — are not tested enough,” Pokrovsky says.
68% of new HIV infections in Russia were the result of heterosexual sexual contact,
so sex education is needed to combat the epidemic.
Pokrovsky argues that to effectively combat the epidemic, the Russian government should promote sex education and fund social advertising campaigns.
“Nowadays, the biggest chunk of funding, over 30 billion rubles [per year], is spent on procuring drugs,” he says. “Treatment is supported by the pharmaceutical companies, so that is where the bulk of the funds are allocated. But there are no market-based solutions to prevention. In this case, you can only count on public funds. Very little is allocated for prevention, literally 500 million rubles [per year], and this amount does not grow from year to year. Most of it is spent on appeals to get tested, rather than on teaching people how not to get infected with HIV. Sex education is now practically prohibited [in Russia].”
Russia was among the top five countries in terms of new HIV case numbers in 2021. According to UNAIDS (the United Nations HIV/AIDS program), Russia accounted for 3.9% of the one and a half million new cases of infection in the world. Russia was bested, in 2021, only by South Africa (14% of all new cases), Mozambique (6.5%), Nigeria (4.9%), and India (4.2%). The Russian Foreign Ministry dubbed the news a “dirty information campaign” on the part of the West. Instead of receiving support, many Russian NGOs campaigning for HIV prevention and patient care have been labeled “foreign agents” by the Russian authorities.
Contrary to the stereotype that drug addicts are the most infected segment of the populace, heterosexual sexual contact is now the primary mode of HIV transmission in Russia, accounting for 68% of new cases.
You can take an HIV test free of charge and anonymously at AIDS centers in all regions of the country.
Source: “Every third region of Russia is experiencing a third-stage HIV epidemic. But the authorities refuse to recognize the growth of infections and purchase the medicines needed. Cutting-edge drugs are available to patients only in the wealthiest regions,” Important Stories (IStories), 13 April 2023. Translated by the Russian Reader
In Russian prisons, they said they were deprived of effective treatments for their H.I.V. On the battlefield in Ukraine, they were offered hope, with the promise of anti-viral medications if they agreed to fight.
It was a recruiting pitch that worked for many Russian prisoners.
About 20 percent of recruits in Russian prisoner units are H.I.V. positive, Ukrainian authorities estimate based on infection rates in captured soldiers. Serving on the front lines seemed less risky than staying in prison, the detainees said in interviews with The New York Times.
“Conditions were very harsh” in Russian prison, said Timur, 37, an H.I.V.-positive Russian soldier interviewed at a detention site in the city of Dnipro in central Ukraine, and identified only by a first name, worried that he would face retaliation if he returned to Russia in a prisoner swap.
After he was sentenced to 10 years for drug dealing, the doctors in the Russian prison changed the anti-viral medication he had been taking to control H.I.V. to types he feared were not effective, Timur said.
He said he did not think he could survive a decade in Russian prison with H.I.V. In December, he agreed to serve six months in the Wagner mercenary group in exchange for a pardon and supplies of anti-viral medications.
“I understood I would have a quick death or a slow death,” he said of choosing between poor H.I.V. treatment in prison and participating in assaults in Russia’s war in Ukraine. “I chose a quick death.”
[…]
 “#Hangers for the Health Ministry,” “Give us a choice,” “Without state-funded abortions there will be backroom abortions,” “The Health Ministry violates human rights,” “Banning abortions is no solution”: a protest installation set up by feminists outside of Hospital No. 1 in Chelyabinsk. Photo by Anastasia Zelentsova. Courtesy of
“#Hangers for the Health Ministry,” “Give us a choice,” “Without state-funded abortions there will be backroom abortions,” “The Health Ministry violates human rights,” “Banning abortions is no solution”: a protest installation set up by feminists outside of Hospital No. 1 in Chelyabinsk. Photo by Anastasia Zelentsova. Courtesy of  Russia has an HIV epidemic. According to the
Russia has an HIV epidemic. According to the